Sickle Cell Disease is a genetic blood disorder that affects millions of people worldwide. According to the Centers for Disease Control and Prevention, Sickle Cell Disease affects about 100,000 people in the US, with African Americans being disproportionately affected. It is a debilitating condition that can cause severe pain and other complications. Despite the advancements in modern medicine, sickle cell disease still continues to affect a considerable number of people in various regions. In this article, we will dive deep into the causes, symptoms, and treatment of sickle cell disease.
Causes
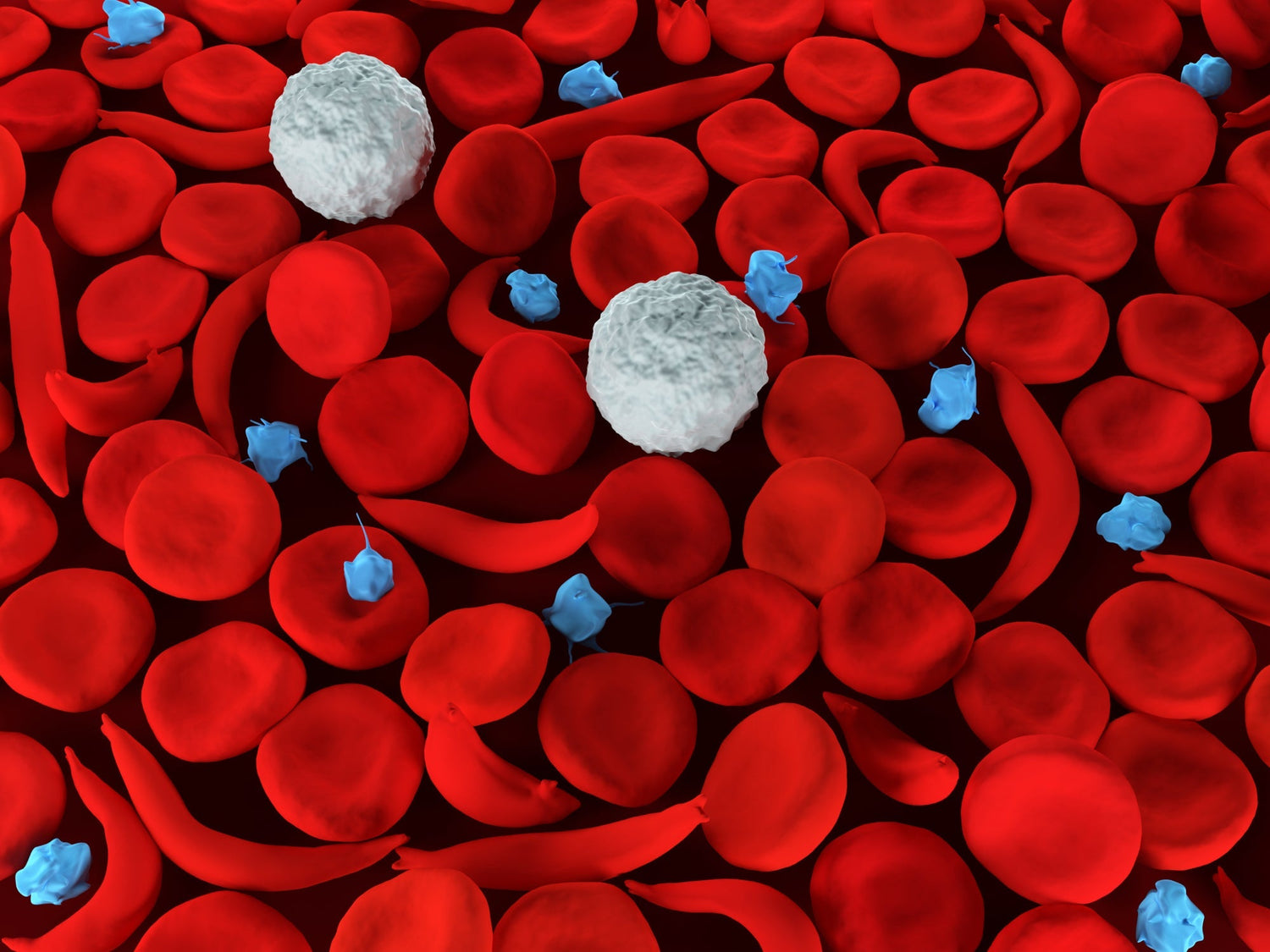
Sickle cell disease is caused by a genetic mutation that affects the production of hemoglobin in red blood cells1. Hemoglobin is the protein in the red blood cells that carries oxygen to different parts of the body. The genetic mutation causes the red blood cells to develop an unusual sickle shape, making them sticky and less flexible. These sickle-shaped cells clog the blood vessels, leading to reduced blood flow and oxygen supply to different organs in the body.
Symptoms
Symptoms of sickle cell disease can vary from person to person. The most common symptoms include severe pain, fatigue, increased susceptibility to infections, delayed growth and development, and swelling of the feet and hands. In severe cases, it can also cause organ damage, stroke, and chronic anemia. People with sickle cell disease often experience acute episodes of severe pain called crisis, which can last for several days and require hospitalization.
Treatment
Although there is no known cure for sickle cell disease, there are several treatments available that can help manage the symptoms and complications of the condition. The treatment starts with managing pain, usually through pain medications or blood transfusion. Antibiotics can also help prevent infections, and hydroxyurea can be used to reduce the frequency of crises. In severe cases, bone marrow or stem cell transplant can also be considered.
Coping with sickle cell disease
Coping with sickle cell disease can be challenging, both for the people living with the condition and their families. It is essential to maintain a healthy lifestyle by staying active, eating a healthy diet, and drinking plenty of water. It is also crucial to manage stress and fatigue, which can trigger a crisis. Finally, it is essential to have a support system in place, including doctors, therapists, and support groups, to help deal with the challenges of living with sickle cell disease.
Research and future outlook
There have been significant advancements in sickle cell disease research2, with several new treatments currently in development. Gene therapy, which involves modifying the genetic mutation causing sickle cell, is one of the most promising avenues of treatment. Clinical trials are currently underway, and if successful, it could provide a permanent cure for sickle cell disease. In the future, we can expect more advancements that would significantly improve the lives of people with sickle cell disease.
Sickle Cell Disease is a complex and challenging condition that affects millions of people worldwide. While there are several treatments available, most are designed to manage the symptoms rather than curing the condition. Coping with sickle cell disease requires a comprehensive approach that involves maintaining a healthy lifestyle, managing stress, and having a support system in place. Despite the challenges, there is hope for the future, with several promising treatments currently under development. By raising awareness and supporting research, we can move towards a future where sickle cell disease is a thing of the past.
References
National Heart, Lung, and Blood Institute. (n.d.). Sickle Cell Disease. Retrieved May 3, 2023, from https://www.nhlbi.nih.gov/health/sickle-cell-disease
Nienhuis, A. W., & Persons, D. A. (2021). Gene therapy for sickle cell disease: Where we are. Hematology, 2021(1), 174-182. https://doi.org/10.1182/hematology.2020000139




Leave a comment
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.